By Stuart Foxman
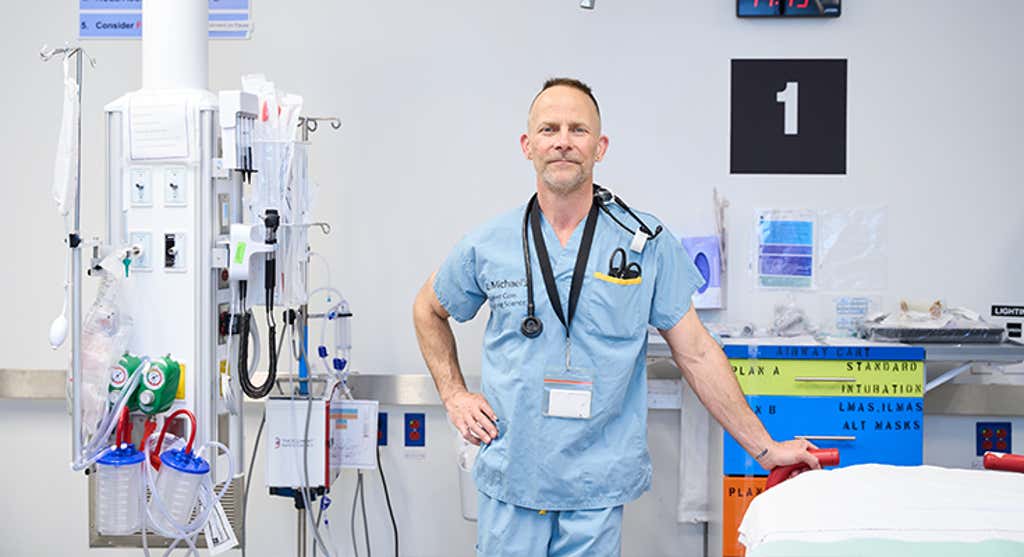
Is burnout just an occupational hazard in medicine? It shouldn’t be, says Dr. James Maskalyk, an emergency physician at St. Michael’s Hospital in Toronto. Being a doctor is a busy, high-pressure job, but it also has rewards like few others.
“The work we do is special. The ER is a sacred place. A special type of humanity is evoked here,” says Dr. Maskalyk.
In January, he was appointed Wellness Director for the Divisions of Emergency Medicine at the University of Toronto. He aims to establish a network of physicians acting as “wellness leads” in the day-to-day work of the emergency medicine departments. The physician-wellness leads will liaise with staff and bring forward possible changes, such as creating a quiet room where staff can take some time to just catch their breath and be with their thoughts.

Working together, Dr. Maskalyk believes colleagues can nurture a deeper culture of well-being.
“My objective for well-being is you look forward to going into work most days,” he says.
Dr. Maskalyk's goal sounds modest, but it could have genuine impact in addressing one of the biggest issues facing physician wellness.
The Canadian Medical Association’s National Physician Health Survey found more than half of physicians and medical learners (53 percent) experienced high levels of burnout. That compared to 30 percent in a similar 2017 survey. Moreover, nearly half (46 percent) of Canadian physicians who responded said they were considering reducing their clinical work in the next 24 months.
Burnout can be defined as a psychological state of emotional exhaustion, depersonalization and a reduced sense of accomplishment. It takes a personal and professional toll and poses a patient safety risk in terms of possibly diminished care, reduced access to care, increased errors and all of the adverse outcomes that can result.
“These are opportunities to metabolize what’s coming up, as close to the incident as possible, so the echoes don’t start to affect you.”
Emergency medicine has been especially hard hit by burnout, and its left many practitioners considering a move to a less stressful area of practice. In the ER, Dr. Maskalyk says doctors are constantly dealing with their patients’ worst days, which can be emotionally taxing. “We were taught stoicism and compartmentalization. It’s tough to heal alone. We heal best in community.”
So, Dr. Maskalyk focuses on interventions, like critical incident debriefing. In a recent one, he shared with his colleagues that the idea wasn’t to get into the nuts and bolts of what occurred, but how they all felt when things didn’t go as desired.
Another practice he hopes to spread is called “the pause” — taking a moment after a patient’s death or other trauma to reflect on the person, the event and the efforts of the medical team. “These are opportunities to metabolize what’s coming up, as close to the incident as possible, so the echoes don’t start to affect you. Burnout are these stresses from work that creep into your life, making you question the utility of work.” Other aspects of enhancing wellness can include peer support and mindfulness training.
Dr. Maskalyk says you can look at the rising levels of burnout in two ways: the end is near or we’re developing the vocabulary for something that has existed for some time.
“Burnout is here and we all touch it at certain points.”
Many factors contribute to burnout, including excessive workloads, growing patient complexity, administrative burdens, lack of organizational support, and shortcomings in the broader health and social services system (which can drive up patient visits).
“There’s no difference for me. I’m a past patient and a future patient, and just temporarily in a white coat.”
Addressing systemic factors is critical. Much is beyond the control of any individual doctor, but some critically important things are - such as the atmosphere in which they work and the communications they have with each other. In a piece for Toronto Life earlier this year about how he’s working to address burnout, Dr. Maskalyk wrote, “I know having supportive colleagues can make all the difference in times of crisis.”
He was referring to his own diagnosis of stage-four thyroid cancer in 2020, and how his colleagues covered his shifts and even offered to help him financially when he was off work. You need to be held by a community of people who care about you, he wrote.
That’s true whether dealing with a health crisis or managing the stresses of the job. Dr. Maskalyk also doesn’t separate the impacts of burnout on the doctors and, by extension, their patients. “There’s no difference for me. I’m a past patient and a future patient, and just temporarily in a white coat.”
Wellness initiatives at the local level may have their limitations. You can treat the symptoms of burnout, but also have to get at the root cause to avoid the spread. “Both have to occur,” affirms Dr. Maskalyk, who in 2022, became executive editor-in chief of the Canadian Medical Association Journal.
The burnout discussion is part of a much bigger question, he says: “Is the health care system as it’s designed now tenable? If a hospital works well, we don’t need a wellness program.”
Dr. Anil Chopra says Dr. Maskalyk’s work is a lifeline for emergency physicians like himself. “There is currently a pervasive sense of helplessness, emotional exhaustion, compassion fatigue and depersonalization in the emergency medicine system, where physicians don’t see a ray of hope on the horizon. We need individuals like Dr. Maskalyk to champion collective strategies to improve physician wellbeing," says Dr. Chopra, who is also the Division Director of Emergency Medicine, Department of Medicine, University of Toronto, and a medical advisor at CPSO.
There’s no single or simple way to stem or manage burnout, but Dr. Maskalyk is intent on changing the culture so physicians have the encouragement and opportunity to express vulnerability and ask for help.
He also has one crucial piece of advice for colleagues: “Find the parts of the work you love the most and bring them ever closer.”













